Navigating the world of dental insurance can sometimes feel like deciphering a foreign language. With…

Visit a Dentist— ANY Dentist
The Member Group Comprehensive PPO is a dental plan that can help you save1 and get the care you need.
No matter who your dentist may be, with the MetLife Preferred Dentist Program, the power to choose and save is yours.
Here are the facts:
- You can go to any licensed dentist, in or out of the network.
- Reimbursement for your out-of-network dental care is based on the 90th percentile of “reasonable and customary” charges1. We look at what dentists in your area actually charge for services, and we calculate reimbursement based on the 90th percentile of those charges.
- The way we determine allowable charges for the 90th R&C means your eligible benefit amount for out-of-network care is high relative to average dental charges in the community. This helps you pay less out of pocket.
- Sometimes when you visit an out-of-network dentist you may have to pay part of the bill. This is called balance billing. But with a 90th percentile R&C plan, in most cases, you won’t be balance billed above your typical out-of-pocket costs – your deductible, coinsurance amount, and your plan maximum.
Take charge of your dental care
Talk to your dentist
Before you get any major dental work, you should talk to your dentist about getting a pretreatment estimate2. That’s when your dentist sends the plan for your care to MetLife.
For most procedures, you and your dentists will receive the estimate – online or by fax – during your visit. The statement shows amounts for what your plan covers. Then you and your dentist can talk about your care and costs before your treatment. It’s a great way to be prepared and plan ahead.
Get your plan information – fast!
Managing your dental benefits has never been easier. You’ve got MyBenefits – your secure member website. Just log on at www.metlife.com/mybenefits. With the 24/7 website you can3:
- Review your plan information, including what’s covered and coinsurance
- Track your deductible and plan maximums
- Find a dentist or view your claim history
- Read up on the oral health information you need to make informed decisions about your care
Take a look at the charts below. They will give you a better idea of how your plan works when you visit a participating (in-network) or a non-participating (out-of-network) dentist.
The 90th bar
This chart shows how often plan members across the nation usually go to a participating or non-participating dentist. It also shows just how rare it is for you to pay more than your typical out-of-pocket costs.
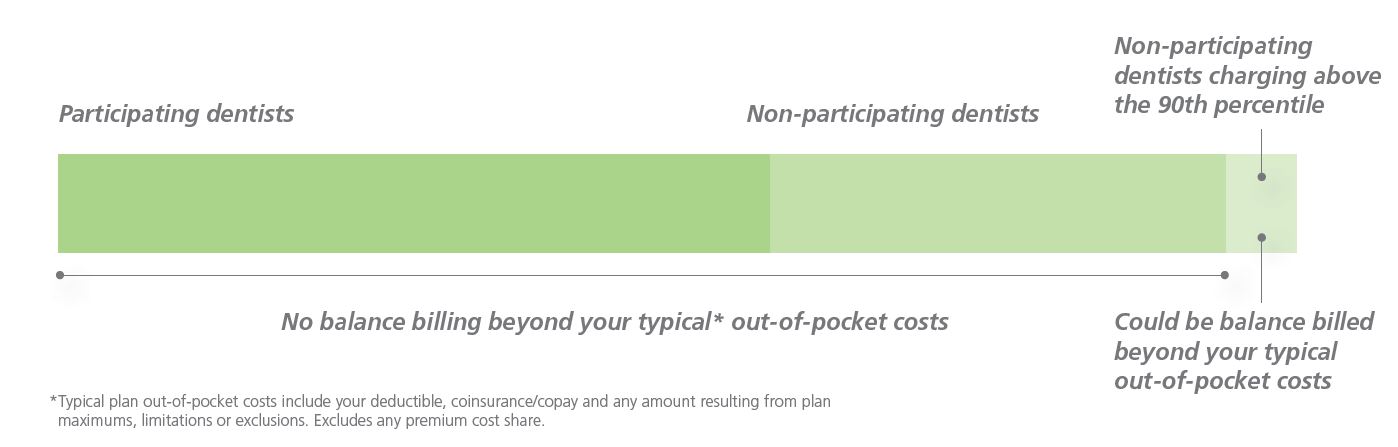 Savings example
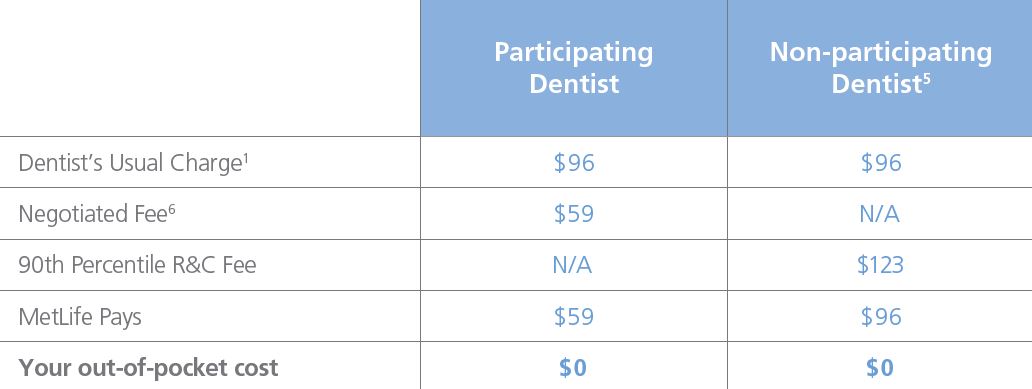
Savings example
This hypothetical example shows that whether you get a cleaning from a participating or non-participating dentist, you can still save money4.
 Visit any licensed dentist. The choice is all yours!
Visit any licensed dentist. The choice is all yours!
Like most group benefit programs, benefit programs offered by MetLife and its affiliates contain certain exclusions, exceptions, waiting periods, reductions of benefits, limitations, and terms for keeping them in force. Please contact MetLife or your Plan Administrator for complete details.
For more information, please click here.
1R&C fee refers to the Reasonable and Customary (R&C) charge, which is based on the lowest of 1) the dentist’s actual charge, 2) the dentist’s usual charge for the
same or similar services or the usual charge of most dentists in the same geographic area for the same or similar services as determined by MetLife.
2Actual benefit determinations are made when services are rendered and are subject to the following as applicable on the date of service: patient eligibility; plan and frequency limitations; maximums and deductibles; and other coverages.
3With the exception of scheduled or unscheduled systems maintenance or interruptions, the MyBenefits website is typically available 24 hours a day, 7 days a week.
4Please note: This is a hypothetical example that reviews an adult teeth cleaning (D1110) in the Chicago area, zip 60601. It assumes that the annual deductible has been met.
5This example excludes non-participating dentists who charge more than what 90% of what other dentists in the area charge. Please note that if you receive care from a dentist that falls into this category, your out-of-pocket costs may be higher.
6Negotiated Fee refers to the fees that in-network dentists have agreed to accept as payment in full, subject to any co-payments, deductibles, cost sharing and benefits maximums.


